Osteoarthritis is the most typical form of arthritis, impacting millions of individuals worldwide. It occurs when the protective cartilage on the ends of your bones uses down with time.
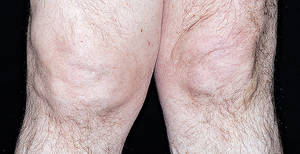
Although osteoarthritis can harm any joint in your body, the condition most typically influences joints in your hands, knees, hips and spinal column.
Osteoarthritis typically gradually gets worse, and no cure exists. However remaining active, keeping a healthy weight and other treatments may slow progression of the disease and assistance improve pain and joint function.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Symptoms of Osteoarthritis
Osteoarthritis symptoms typically establish slowly and worsen in time. Signs and symptoms of osteoarthritis consist of:
- Pain. Your joint might injure during or after movement.
- Tenderness. Your joint may feel tender when you apply light pressure to it.
- Tightness. Joint stiffness may be most visible when you get up in the early morning or after a period of inactivity.
- Loss of versatility. You might not be able to move your joint through its complete variety of motion.
- Grating sensation. You may hear or feel a grating feeling when you use the joint.
- Bone spurs. These extra little bits of bone, which feel like difficult swellings, may form around the affected joint.
When to see a doctor
If you have joint pain or tightness that lasts for more than a few weeks, make a visit with your doctor.
Causes of Osteoarthritis
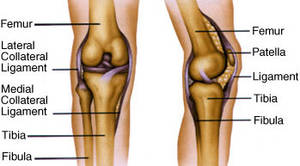
Osteoarthritis occurs when the cartilage that cushions the ends of bones in your joints gradually deteriorates. Cartilage is a firm, slippery tissue that permits almost smooth joint motion. In osteoarthritis, the slick surface area of the cartilage ends up being rough. Eventually, if the cartilage wears down completely, you may be left with bone rubbing on bone.
Risk factors
Factors that may enhance your risk of osteoarthritis consist of:
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
- Older age. The risk of osteoarthritis increases with age.
- Sex. Women are most likely to develop osteoarthritis, though it isn’t clear why.
- Obesity. Carrying extra body weight contributes to osteoarthritis in several methods. It puts included stress on weight-bearing joints, such as your hips and knees. In addition, fat tissue produces proteins that may cause dangerous inflammation around your joints.
- Joint injuries. Injuries, such as those that occur when playing sports or from a mishap, may increase the risk of osteoarthritis.
- Specific professions. If your job includes jobs that position repeated stress on a particular joint, that joint might ultimately develop osteoarthritis.
- Genes. Some people inherit a tendency to develop osteoarthritis.
- Bone defects. Some individuals are born with malformed joints or malfunctioning cartilage, which can enhance the risk of osteoarthritis.
- Other diseases. Having diabetes or other rheumatic diseases such as gout and rheumatoid arthritis can enhance your risk of osteoarthritis.
Problems & Complications
Osteoarthritis is a degenerative disease that gets worse over time. Joint pain and stiffness might end up being severe sufficient making daily jobs difficult. Some individuals are not able to work. When joint pain is this severe, doctors may recommend joint replacement surgery.
Tests and diagnosis
During the physical exam, your doctor will carefully examine your influenced joint, looking for inflammation, swelling or inflammation, and for range of motion in the joint. Your doctor may also suggest imaging and lab tests
Imaging tests
Images of the affected joint can be obtained during imaging tests. Examples consist of:
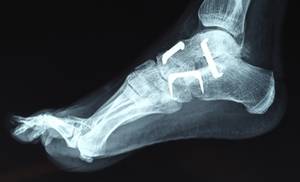
- X-rays. Cartilage doesn’t show up on X-ray images, however cartilage loss is revealed by a constricting of the area in between the bones in your joint. An X-ray may also show bone spurs around a joint. Some individuals may have X-ray evidence of osteoarthritis prior to they experience any symptoms.
- Magnetic resonance imaging (MRI). MRI utilizes radio waves and a strong electromagnetic field to produce in-depth pictures of bone and soft tissues, including cartilage. MRI isn’t commonly had to diagnose osteoarthritis but may help supply more information in complicated cases.
Laboratory tests
Examining your blood or joint fluid can assist identify the medical diagnosis.
Blood tests. Blood tests might help dismiss other causes of joint pain, such as rheumatoid arthritis.
Joint fluid analysis. Your doctor might use a needle to draw fluid out of the affected joint. Analyzing and testing the fluid from your joint can identify if there’s swelling and if your pain is caused by gout or an infection.
Treatments for Osteoarthritis
There’s no known remedy for osteoarthritis, however treatments can help in reducing pain and preserve joint movement.
Medications
Osteoarthritis symptoms might be assisted by certain medications, consisting of:
- Acetaminophen. Acetaminophen (Tylenol, others) can relieve pain, but it does not minimize inflammation. It has been revealed to be efficient for people with osteoarthritis who have mild to moderate pain. Taking more than the advised dose of acetaminophen can cause liver damage.
- Nonsteroidal anti-inflammatory drugs (NSAIDs). NSAIDs may reduce swelling and eliminate pain. Over-the-counter NSAIDs include ibuprofen (Advil, Motrin IB, others) and naproxen (Aleve, others). Stronger NSAIDs are readily available by prescription. NSAIDs can cause stomach upset, sounding in your ears, cardiovascular problems, bleeding problems, and liver and kidney damage. They ought to not be utilized by individuals over 65 years of age and those who have stomach bleeding. Topical NSAIDS have less side effects and may ease pain simply as well.
Therapy
Working out and achieving a healthy weight are the best and most important ways to alleviate osteoarthritis. Your doctor likewise might recommend:
- Physical therapy. A physiotherapist can work with you to produce a customized exercise program that will enhance the muscles around your joint, enhance your variety of movement and reduce pain.
- Occupational therapy. An occupational therapist can assist you find methods to do daily tasks or do your job without putting extra stress on your currently painful joint. For example, a toothbrush with a large grip could make brushing your teeth simpler if you have finger osteoarthritis. A bench in your shower might assist ease the pain of standing if you have knee osteoarthritis.
- Braces or shoe inserts. Your doctor may advise shoe inserts or other devices that can help in reducing pain when you stand or walk. These devices can debilitate or promote your joint to assist take pressure off it.
- A chronic pain class. The Arthritis Foundation and some medical centers have classes for individuals with osteoarthritis and chronic pain. Ask your doctor about classes in your area or check with the Arthritis Foundation. These classes teach skills that help you handle your osteoarthritis pain. And you’ll meet other people with osteoarthritis and learn their tips and techniques for reducing and managing joint pain.
Surgical and other procedures
If conservative treatments don’t assist, you might wish to consider treatments such as:
- Cortisone shots. Injections of corticosteroid medications may ease pain in your joint. During this procedure your doctor numbs the area around your joint, then places a needle into the area within your joint and injects medication. The number of cortisone shots you can get each year is limited, because the medication can aggravate joint damage with time.
- Lubrication injections. Injections of hyaluronic acid might offer pain relief by supplying some cushioning in your knee. Hyaluronic acid resembles an element normally discovered in your joint fluid.
- Realigning bones. During a surgery called an osteotomy, the surgeon crosses the bone either above or below the knee to realign the leg. Osteotomy can decrease knee pain by shifting your body weight away from the worn-out part of your knee.
- Joint replacement. In joint replacement surgery (arthroplasty), your specialist removes your broken joint surface areas and replaces them with plastic and metal parts. The hip and knee joints are those most typically changed. Surgical risks consist of infections and embolism. Artificial joints can wear or come loose and may need to become replaced. Repeat joint replacements are more tough and less effective than the initial surgery.
Lifestyle and home remedies
Lifestyle modifications and home treatments also can help in reducing osteoarthritis symptoms. You may wish to try some of the following tips:
- Workout. Exercise can increase your endurance and strengthen the muscles around your joint, making your joint more steady. Try walking, biking or swimming. If you feel new joint pain, stop. New pain that lasts for hours after you work out probably suggests you’ve overdone it however doesn’t mean you need to stop working out entirely.
- Slim down. Being overweight or obese boosts the stress on your weight-bearing joints, such as your knees and your hips. Even a percentage of weight loss can relieve some pressure and reduce your pain. Talk to your doctor about healthy methods to drop weight. Many people integrate modifications in their diet with enhanced workout.
- Use cold and heat to manage pain. Both heat and cold can alleviate pain in your joint. Heat likewise eases tightness, and cold can ease muscle spasms and pain.
- Apply over the counter pain creams. Creams and gels readily available at pharmacies may offer temporary relief from osteoarthritis pain. Some creams numb the pain by producing a hot or cool experience. Other creams consist of medications, such as aspirin-like compounds, that are taken in into your skin. Pain creams work best on joints that are close to the surface area of your skin, such as your knees and fingers.
- Usage assistive devices. Assistive devices can make it simpler to set about your day without stressing your painful joint. A walking cane may take weight off your knee or hip as you walk. Bring the cane in the hand opposite the leg that injures. Clutching and getting hold of tools might make it much easier to work in the cooking area if you have osteoarthritis in your fingers. Your doctor or occupational therapist may have ideas about what sorts of assistive devices might be handy to you. Brochures and medical supply shops likewise might be locations to try to find ideas.