Knee pain is a typical complaint that impacts people of all ages. Knee pain may be the result of an injury, such as a burst ligament or torn cartilage. Medical conditions– consisting of arthritis, gout and infections– also can cause knee pain.
Lots of types of small knee pain respond well to self-care steps. Physical therapy and knee braces also can help alleviate knee pain. In some cases, however, your knee may require medical repair.
Symptoms of Knee Pian
The area and seriousness of knee pain may vary, depending upon the reason for the problem. Signs and symptoms that in some cases accompany knee pain include:
- Swelling and tightness
- Soreness and heat to the touch
- Weak point or instability
- Popping or crunching sounds
- Inability to totally straighten the knee
Knee pain: when to see a doctor
Call your doctor if you:
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
- Can’t bear weight on your knee
- Have significant knee swelling
- Are unable to completely extend or flex your knee
- See an evident deformity in your leg or knee
- Have a fever, in addition to redness, pain and swelling in your knee
- Feel as if your knee is unsteady or your knee “gives out”.
What Causes a Knee Pain?
Knee pain can be triggered by injuries, mechanical issues, types of arthritis and other issues.
Knee Injuries
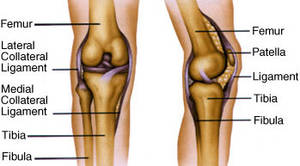
A knee injury can affect any of the ligaments, tendons or fluid-filled sacs (bursae) that surround your knee joint in addition to the bones, cartilage and ligaments that form the joint itself. A few of the more common knee injuries include:
- ACL injury. An ACL injury is the tearing of the anterior cruciate ligament (ACL)– among 4 ligaments that connect your shinbone to your thighbone. An ACL injury is particularly typical in people who play basketball, soccer or other sports that require abrupt changes in direction.
- Fractures. The bones of the knee, including the kneecap (patella), can be broken during motor vehicle collisions or falls. People whose bones have actually been deteriorated by osteoporosis can often sustain a knee fracture merely by stepping incorrect.
- Torn meniscus. The meniscus is formed of hard, rubbery cartilage and acts as a shock absorber in between your shinbone and thighbone. It can be torn if you suddenly twist your knee while bearing weight on it.
- Knee bursitis. Some knee injuries cause swelling in the bursae, the little sacs of fluid that cushion the beyond your knee joint so that tendons and ligaments glide efficiently over the joint.
- Patellar tendinitis. Tendinitis is irritation and swelling of several tendons– the thick, fibrous tissues that attach muscles to bones. Runners, skiers, cyclists, and those involved in jumping sports and activities are susceptible to develop inflammation in the patellar tendon, which links the quadriceps muscle on the front of the thigh to the shinbone.
Mechanical issues
Some examples of mechanical issues that can cause knee pain consist of:.
- Loose body. Often injury or degeneration of bone or cartilage can cause a piece of bone or cartilage to break off and drift in the joint area. This may not produce any problems unless the loose body hinders knee joint motion, where case the result is something like a pencil captured in a door hinge.
- Iliotibial band syndrome. This takes place when the difficult band of tissue that extends from the outside of your hip to the beyond your knee (iliotibial band) becomes so tight that it rubs versus the outer part of your femur. Distance runners are specifically susceptible to iliotibial band syndrome.
- Dislocated kneecap. This happens when the triangular bone (patella) that covers the front of your knee slips out of place, typically to the beyond your knee. In many cases, the kneecap may remain displaced and you’ll be able to see the dislocation.
- Hip or foot pain. If you have hip or foot pain, you may change the way you walk to spare these painful joints. But this altered gait can position more stress on your knee joint. Sometimes, problems in the hip or foot can refer pain to the knee.
Types of arthritis
More than 100 different types of arthritis exist. The ranges more than likely to affect the knee include:.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
- Osteoarthritis. Sometimes called degenerative arthritis, osteoarthritis is the most typical type of arthritis. It’s a wear-and-tear condition that happens when the cartilage in your knee deteriorates with usage and age.
- Rheumatoid arthritis. The most devastating type of arthritis, rheumatoid arthritis is an autoimmune condition that can influence nearly any joint in your body, including your knees. Although rheumatoid arthritis is a chronic disease, it has the tendency to vary in intensity and may even come and go.
- Gout. This kind of arthritis happens when uric acid crystals develop in the joint. While gout most commonly impacts the big toe, it can also take place in the knee.
- Pseudogout. Typically incorrect for gout, pseudogout is caused by calcium-containing crystals that develop in the joint fluid. Knees are the most common joint influenced by pseudogout.
- Septic arthritis. In some cases your knee joint can end up being infected, leading to swelling, pain and redness. There’s usually no injury before the onset of pain. Septic arthritis frequently accompanies a fever.
Other problems
Patellofemoral pain syndrome is a general term that refers to pain occurring between your patella and the underlying thighbone (femur). It’s typical in athletes; in young people, especially those who have a slight maltracking of the kneecap; and in older adults, who typically develop the condition as a result of arthritis of the kneecap.
Risk factors
A number of elements can enhance your risk of having knee problems, including:.
- Excess weight. Being overweight or obese boosts stress on your knee joints, even during regular activities such as walking or going up and down stairs. It also puts you at enhanced risk of osteoarthritis by accelerating the breakdown of joint cartilage.
- Absence of muscle flexibility or strength. A lack of strength and versatility are among the leading causes of knee injuries. Tight or weak muscles provide less support for your knee because they do not soak up enough of the stress put in on the joint.
- Certain sports. Some sports put greater stress on your knees than do others. Alpine snowboarding with its stiff ski boots and prospective for falls, basketball’s jumps and pivots, and the repeated pounding your knees take when you run or jog all enhance your risk of knee injury.
- Previous injury. Having a previous knee injury makes it more likely that you’ll injure your knee again.
Complications
Not all knee pain is major. However some knee injuries and medical conditions, such as osteoarthritis, can lead to enhancing pain, joint damage and impairment if left neglected. And having a knee injury– even a minor one– makes it more likely that you’ll have comparable injuries in the future.
Diagnosis
During the physical examination, your doctor is most likely to:.
- Check your knee for swelling, pain, inflammation, warmth and noticeable bruising.
- Check to see how far you can move your lower leg in different instructions.
- Press on or pull the joint to examine the honesty of the structures in your knee.
Imaging tests for knee
In many cases, your doctor may suggest tests such as:
- X-ray. Your doctor may first suggest having an X-ray, which can assist find bone fractures and degenerative joint disease.
- Computerized tomography (CT) scan. CT scanners integrate X-rays taken from many different angles, to create cross-sectional images of the within your body. CT scans can help identify bone problems and find loose bodies.
- Ultrasound. This technology utilizes acoustic waves to produce real-time images of the soft tissue structures within and around your knee, and how they are working. Your doctor may want to steer your knee into different positions during the ultrasound, to check for specific problems.
- Magnetic resonance imaging. An MRI uses radio waves and a powerful magnet to develop 3-D pictures of the within your knee. This test is particularly helpful in revealing injuries to soft tissues such as ligaments, tendons, cartilage and muscles.
Laboratory tests
If your doctor believes an infection, gout or pseudogout, you’re most likely to have blood tests and sometimes arthrocentesis, a procedure in which a small amount of fluid is removed from within your knee joint with a needle and sent out to a laboratory for analysis.
Treatment for Knee Pain
Treatments will differ, depending upon what exactly is causing your knee pain.
Medications
Your doctor might recommend medications to assist relieve pain and to treat underlying conditions, such as rheumatoid arthritis or gout.
Therapy
Enhancing the muscles around your knee will make it more stable. Training is likely to concentrate on the muscles on the front of your thigh (quadriceps) and the muscles in the back of your thigh (hamstrings). Fixing suboptimal motion patterns is also useful, along with developing excellent technique during your sport or activity. Exercises to enhance your balance likewise are important.
Arch promotes, often with wedges on one side of the heel, can help to move pressure far from the side of the knee most influenced by osteoarthritis. In specific conditions, various types of braces may be utilized to help secure and support the knee joint.
Injections for Knee Pain
Sometimes, your doctor might recommend injecting medications or other substances directly into your joint. Examples include:
- Corticosteroids. Injections of a corticosteroid drug into your knee joint might help in reducing the symptoms of an arthritis flare and supply pain relief that lasts a few months. These injections aren’t reliable in all cases.
- Hyaluronic acid. A thick fluid, much like the fluid that naturally oils joints, hyaluronic acid can be injected into your knee to enhance mobility and ease pain. Although research study results have been mixed about the effectiveness of this treatment, remedy for one or a series of shots may last as long as 6 months.
- Platelet-rich plasma (PRP). PRP includes a concentration of several development elements that appear to decrease inflammation and promote healing. These types of injections have the tendency to work much better in younger individuals and in individuals with mild arthritis.
Surgery
If you have an injury that might need surgery, it’s generally not needed to have the operation instantly. Prior to making any decision, consider the advantages and disadvantages of both nonsurgical rehab and medical restoration in relation to what’s most important to you. If you choose to have surgery, your alternatives might include:.
- Arthroscopic surgery. Depending upon your injury, your doctor may have the ability to examine and fix your joint damage using a fiber-optic cam and long, narrow tools inserted through just a few little incisions around your knee. Arthroscopy might be used to get rid of loose bodies from your knee joint, eliminate or fix damaged cartilage (especially if it is causing your knee to lock), and rebuild torn ligaments.
- Partial knee replacement surgery. In this procedure (unicompartmental arthroplasty), your cosmetic surgeon replaces just the most damaged portion of your knee with parts made from metal and plastic. The surgery can usually be carried out through little cuts, so you’re likely to recover more quickly than you are with surgery to change your whole knee.
- Overall knee replacement. In this procedure, your specialist cuts away harmed bone and cartilage from your thighbone, shinbone and kneecap, and replaces it with an artificial joint made from metal alloys, top-quality plastics and polymers.